Every mother hopes for a simple, uncomplicated pregnancy. But the process of growing a baby is anything but easy, creating ample opportunity for things to go awry. While there often isn’t much we can do to prevent complications, being aware of the warning signs can be lifesaving.
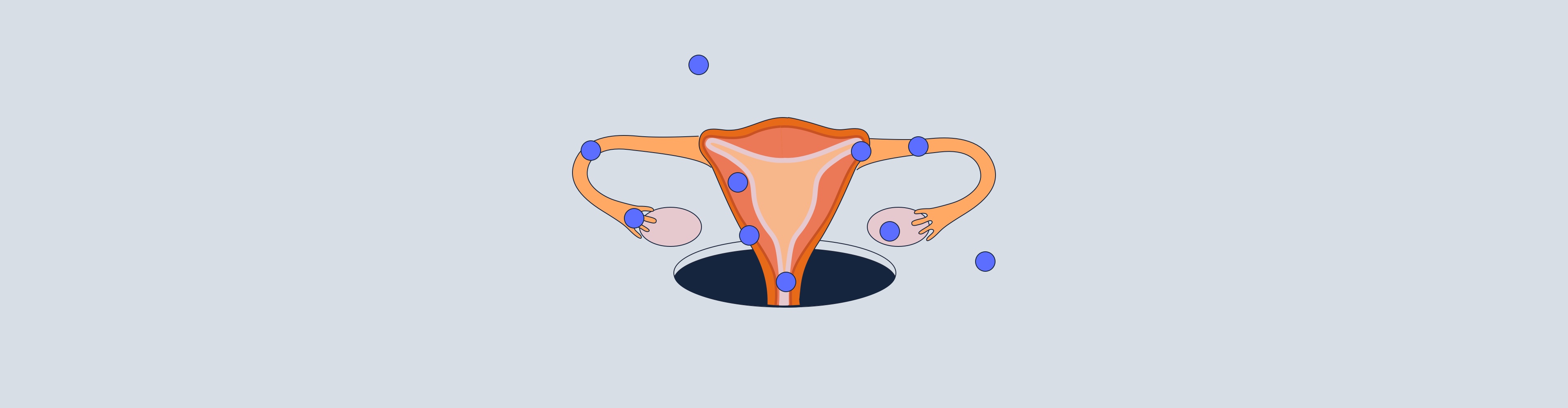
In a normal pregnancy, sperm fertilises the egg which then travels from the ovary through the fallopian tube and into the uterus where it attaches itself to the uterine wall and begins to grow into a baby along with the placenta. An ectopic pregnancy occurs during this first part of pregnancy, soon after fertilisation of the egg.
What is it?
In Greek, the word 'ectopic' means 'out of place', and that's exactly what happens during an ectopic pregnancy [3]. Instead of attaching to the lining of the uterus, the embryo implants where it isn't supposed to. There are a couple of different places it can do this:
- Ovary - where the eggs are produced and fertilised
- Fallopian Tube - the tube between the ovary and uterus. This is the most common place for ectopic pregnancies, and implantation can happen anywhere along the tube [4].
- Cervix - the exit point below the uterus
- Intra-abdominal region - outside of the reproductive organs where the digestive organs are.
Unfortunately, an ectopic pregnancy is almost never viable; however, in extremely rare cases the fetus might survive [5]. The baby and placenta need to be in the uterus to receive a steady supply of blood and nutrients, and plenty of room to grow and develop.
So, are we talking about super rare exceptions, or is an ectopic pregnancy likely to happen to you or a loved one? The rate in developed countries is between 1-2% of all pregnancies [25]. For women conceiving with the help of fertility treatments, such as in vitro fertilization, there may be a 2-5% risk of the pregnancy being ectopic. Additionally, it is the leading cause of maternal deaths in the first trimester [2].
Causes and risk factors
So why does this happen? The fallopian tubes have tiny hair-like structures called cilia, which propel the embryo away from the ovary and into the uterus, similar to a conveyor belt. If the cilia or any part of the fallopian tube are damaged, the embryo won't be able to make it into the uterus and implants itself into the fallopian tube instead. Though many ectopic pregnancies occur without any of the known risk factors [6], some behaviors and conditions might increase the likelihood:
- Smoking can damage the cilia responsible for moving the embryo through the fallopian tube, causing the egg to travel slower, thereby increasing the risk [7].
- If left untreated, pelvic inflammatory disease can cause scar tissue to build up in the fallopian tubes. This can impede or slow down the journey of the embryo through the tube, and thus increase the likelihood of an ectopic pregnancy. Pelvic inflammatory disease is usually caused by STDs such as chlamydia or gonorrhea.
- Tubal ligation decreases the risk of an ectopic pregnancy along with pregnancy in general, but if a pregnancy does occur or if a reversal was attempted, then the risk of an ectopic pregnancy increases [9].
- Similar to tubal ligation, an intrauterine device, or IUD prevents pregnancies in general, but if they do occur then they are more likely to be ectopic [11,12].
- Fertility treatments, such as in vitro fertilization or intrauterine insemination may increase the risk of an ectopic pregnancy depending on the procedure that is used and the health characteristics of the women who seek these fertility treatments in the first place [1,8].
- An induced abortion or the use of levonorgestrel, also known as plan B, in your past does not increase the risk [13, 14]. However, using levonorgestrel repeatedly during your current cycle for further intercourse has been linked with a higher incidence of ectopic pregnancy.
- Other less common conditions such as salpingitis isthmica nodosa, DES exposure, pelvic or abdominal surgery, and a prior ectopic pregnancy are also known to be risk factors for ectopic pregnancies [10].
Prevention
Some data shows that other factors such as maternal age over 35 years or douching can also be risky when it comes to ectopic pregnancies [10]. While we can't do much about our age, forgoing douching is an easy preventative measure. So what else can we do?
Firstly, we can do our best to quit smoking. Since it isn't easy for most people, it's worth asking for help from a healthcare professional who can recommend various tips and strategies for quitting smoking.
Secondly, get tested and treated for infections, especially STDs such as chlamydia or gonorrhea. These infections can lead to pelvic inflammatory disease(PID). The longer PID is left untreated, the more harm may be done to your reproductive organs. This can further reduce the movement speed of the embryo through the tubes and hence results in a higher likelihood of ectopic pregnancy.
Thirdly, if you're considering sterilisation, consider opting for a procedure with a lower risk of ectopic pregnancy. For example, a total removal of the fallopian tubes has nearly zero risk of an ectopic pregnancy vs. a tubal clip which has a higher risk. There are many types of procedures available, so talk to your doctor about the best one for you.
If you've had a previous ectopic pregnancy or have a condition that might make it more likely, talk to your gynecologist about possible prevention strategies or extra monitoring if you're trying to conceive again.
Warning signs
An ectopic pregnancy is a medical emergency and needs to be recognised and treated as soon as possible. So it's important to know the warning signs in case it happens to you or someone you know.
The reason it can be dangerous is that a fetus growing in the fallopian tube can cause the tube or affected organ to rupture and bleed, which can lead to hypovolemic shock and possibly death.
Unfortunately, the signs may not always be obvious. Up to 9% of women don't have any symptoms at all, and up to 33% of women don't present any medical signs [16]. Additionally, the signs may not always be clear.
Early symptoms
At first, you would experience the signs of a regular pregnancy, including a missed period, a positive pregnancy test, and perhaps breast tenderness or nausea.
As the fertilised egg continues to grow outside the womb, other symptoms may begin to appear. The first signs are often light vaginal bleeding or pelvic pain.
Though less common, other symptoms might be:
- A mass or lump in the lower abdomen
- Nausea
- Vomiting
- Diarrhea.
Emergency symptoms
As the egg grows larger it may cause a rupture. The symptoms might be:
- severe abdominal or pelvic pain
- heavy bleeding
- Shoulder pain
- Abdominal or cervical tenderness
- abdominal distension (a swollen belly)
- lightheadedness
- Fainting
If you or someone you know are experiencing any of these symptoms, it is vital to seek emergency medical attention immediately. A rupture can cause strong bleeding, which is very dangerous and cannot be left untreated.
A helpful indicator of possible ectopic pregnancy is timing. Most ectopic pregnancy symptoms present around 7 weeks after the last menstrual period [15], with the range usually being between 6 and 10 weeks [16].
So if you're sexually active and are experiencing any of the above symptoms, it's worth considering the possibility and seeking prompt medical attention.
Diagnosis
The first step in diagnosing an ectopic pregnancy is with a positive pregnancy test. Afterward, a physician will try to locate the fertilised egg using transvaginal ultrasonography, or USG.
Sometimes the result will be obvious while other times the result may be less clear. In this case, measuring β-hCG, the hormone that is measured in pregnancy tests can be helpful. If β-hCG levels are high, but there is no pregnancy visible in the uterus, that could be an indication of an ectopic pregnancy.
Other conditions might mimic the symptoms of an ectopic pregnancy. Some examples are a miscarriage, ovarian torsion, acute appendicitis, a ruptured ovarian cyst, a kidney stone, and pelvic inflammatory disease [17]. Some of these are also medical emergencies, so if there's any doubt, don't hesitate to seek help.
Treatment
Treatment depends on multiple factors such as the size and placement of the embryo, the β-hCG levels, and the symptoms.
While it’s possible for an ectopic pregnancy to resolve on its own, it’s important for it to be closely monitored by a healthcare professional.
If an ectopic pregnancy is caught early it might be possible to manage it with a medication called methotrexate [18]. This will stop the embryo from growing. The embryo will then either be resorbed by the body or pass with the next menstrual period.
If the embryo is too big or bleeding has already occurred then surgery may be necessary. The method used for the surgery is called laparoscopy. A small incision is made to either remove the embryo from the affected organ or to remove the fallopian tube along with the embryo [16].
What happens next?
After treatment with either methotrexate or surgery, it's normal to feel tiredness, abdominal discomfort, or pain for several weeks. While your β-hCG levels are dropping, you may still feel the usual symptoms of pregnancy and might have irregular periods for a couple of cycles [26].
If you’re planning to conceive again, the good news is that methotrexate does not affect the success rate of fertility or future fertility treatments [13,20]. Also, if the fallopian tube was removed during surgery, it's still possible to become pregnant through the other tube or by using in vitro fertilisation [21]. However, a prior history of infertility is the most telling factor [19]. If it was difficult to conceive before, then that isn't likely to change.
Unfortunately, after one ectopic pregnancy, the chance that another one will occur is higher. This is especially true if a fallopian tube was damaged during surgery or if in vitro fertilisation is used to conceive [24].
If you become pregnant again after going through an ectopic pregnancy, be alert for the warning signs and contact your healthcare professional to confirm that the embryo is developing in the uterus.
Getting through an ectopic pregnancy
Whether or not the pregnancy was planned, experiencing an ectopic pregnancy can be overwhelming and often traumatic for many women. Along with the physical pain and discomfort, it can take time to work through the feelings and emotions. It's important to remember that you're not alone and that there's nothing you could have done otherwise.
It can be helpful to talk to a counselor about the experience to make sense of what happened. Since it can sometimes be difficult to open up about the experience with people who haven't gone through it themselves, online forums can be a valuable resource when it comes to getting support from other women who understand what you're going through.
The process of growing a brand new human being is no small or simple matter. While there are many risks involved, modern medicine has made pregnancy safer than ever before. The best we can do on our part is to inform ourselves so that we can take the best course of action when unexpected complications happen or to seek help and support if they already did.
References
1. Kirk E, Bottomley C, Bourne T (2014). "Diagnosing ectopic pregnancy and current concepts in the management of pregnancy of unknown location". Human Reproduction Update. 20 (2): 250–61. doi:10.1093/humupd/dmt047. PMID 24101604.
2. Tenore JL. Ectopic pregnancy. Am Fam Physician 2000;61:1080-8.
3. Cornog MW (1998). Merriam-Webster's vocabulary uilder. Springfield, Mass.: Merriam-Webster. p. 313. ISBN 9780877799108. Archived from the original on 2017-09-10.
4. Cecchino GN, Araujo Júnior E, Elito Júnior J (September 2014). "Methotrexate for ectopic pregnancy: when and how". Archives of Gynecology and Obstetrics. 290 (3): 417–23. doi:10.1007/s00404-014-3266-9. PMID 24791968. S2CID 26727563.
5. Zhang J, Li F, Sheng Q (2008). "Full-term abdominal pregnancy: a case report and review of the literature". Gynecologic and Obstetric Investigation. 65 (2): 139–41. doi:10.1159/000110015. PMID 17957101. S2CID 35923100.
6. Farquhar CM (2005). "Ectopic pregnancy". Lancet. 366 (9485): 583–91. doi:10.1016/S0140-6736(05)67103-6. PMID 16099295. S2CID 26445888.
7. Lyons RA, Saridogan E, Djahanbakhch O (2006). "The reproductive significance of human Fallopian tube cilia". Human Reproduction Update. 12 (4): 363–72. doi:10.1093/humupd/dml012. PMID 16565155.
8. Clayton HB, Schieve LA, Peterson HB, Jamieson DJ, Reynolds MA, Wright VC. Ectopic pregnancy risk with assisted reproductive technology procedures. Obstet Gynecol. 2006 Mar;107(3):595-604. doi: 10.1097/01.AOG.0000196503.78126.62. PMID: 16507930.
9. van Seeters JAH, Chua SJ, Mol BWJ, Koks CAM. Tubal anastomosis after previous sterilization: a systematic review. Hum Reprod Update. 2017 May 1;23(3):358-370. doi: 10.1093/humupd/dmx003. PMID: 28333337.
10. Marion LL, Meeks GR (June 2012). "Ectopic pregnancy: History, incidence, epidemiology, and risk factors". Clinical Obstetrics and Gynecology. 55 (2): 376–86. doi:10.1097/GRF.0b013e3182516d7b. PMID 22510618
11. "ParaGard (copper IUD)". Mayo Clinic. Retrieved 30 November 2018.
12. Kumar V, Gupta J (November 2015). "Tubal ectopic pregnancy". BMJ Clinical Evidence. 2015. PMC 4646159. PMID 26571203.
13. 16 Answering questions about long term outcomes". Management of Unintended and Abnormal Pregnancy: Comprehensive Abortion Care. John Wiley & Sons. 2011. ISBN 9781444358476. Archived from the original on 2017-09-10.
14. Zhang, Jian et al. “Association between levonorgestrel emergency contraception and the risk of ectopic pregnancy: a multicenter case-control study.” Scientific reports vol. 5 8487. 12 Feb. 2015, doi:10.1038/srep08487
15. Tay, J I et al. “Ectopic pregnancy.” The Western journal of medicine vol. 173,2 (2000): 131-4. doi:10.1136/ewjm.173.2.131
16. Sivalingam, Vanitha N et al. “Diagnosis and management of ectopic pregnancy.” The journal of family planning and reproductive health care vol. 37,4 (2011): 231-40. doi:10.1136/jfprhc-2011-0073
17. Crochet JR, Bastian LA, Chireau MV (April 2013). "Does this woman have an ectopic pregnancy?: the rational clinical examination systematic review". JAMA. 309 (16): 1722–9. doi:10.1001/jama.2013.3914. PMID 23613077. S2CID 205049738.
18. Krag Moeller, Lars Bo et al. “Success and spontaneous pregnancy rates following systemic methotrexate versus laparoscopic surgery for tubal pregnancies: a randomized trial.” Acta obstetricia et gynecologica Scandinavica vol. 88,12 (2009): 1331-7. doi:10.3109/00016340903188912
19. Tulandi T, Tan SL, Tan SL, Tulandi T (2002). Advances in Reproductive Endocrinology and Infertility: Current Trends and Developments. Informa Healthcare. p. 240. ISBN 978-0-8247-0844-3.
20. Ohannessian A, Loundou A, Courbière B, Cravello L, Agostini A (September 2014). "Ovarian responsiveness in women receiving fertility treatment after methotrexate for ectopic pregnancy: a systematic review and meta-analysis". Human Reproduction. 29 (9): 1949–56. doi:10.1093/humrep/deu174. PMID 25056087.
21. Fernandez H, Capmas P, Lucot JP, Resch B, Panel P, Bouyer J (May 2013). "Fertility after ectopic pregnancy: the DEMETER randomized trial". Human Reproduction. 28 (5): 1247–53. doi:10.1093/humrep/det037. PMID 23482340.
22. Shawkat E (2005), "Risk Factors for Ectopic Pregnancy”. Best Evidence Topics https://bestbets.org/bets/bet.php?id=921
23. Brady PC (October 2017). "New Evidence to Guide Ectopic Pregnancy Diagnosis and Management". Obstetrical & Gynecological Survey. 72 (10): 618–625. doi:10.1097/OGX.0000000000000492. PMID 29059454.
24. Weigert, Monika et al. “Previous tubal ectopic pregnancy raises the incidence of repeated ectopic pregnancies in vitro fertilization-embryo transfer patients.” Journal of assisted reproduction and genetics vol. 26,1 (2009): 13-7. doi:10.1007/s10815-008-9278-2
25. Panelli DM, Phillips CH, Brady PC. Incidence, diagnosis and management of tubal and nontubal ectopic pregnancies: a review. Fertil Res Pract. 2015 Oct 15;1:15. doi: 10.1186/s40738-015-0008-z. PMID: 28620520; PMCID: PMC5424401.
26. https://www.acog.org/womens-health/faqs/ectopic-pregnancy